Similar insidious frailty and weakness occur in the patients at the end-of-life stage and patients suffering from multisystem chronic diseases such as chronic kidney disease, heart failure, and chronic obstructive pulmonary disease. Weak respiratory and laryngeal musculature can alter sensitivity to aspiration and decrease the drive and strength of the reflexive cough. This, in addition to deconditioning, weak airway muscles, prolonged intubation, and poor airway protection, contribute to an increased risk for significant oropharyngeal dysphagia and aspiration-related pneumonia. 
Critically ill patients with extended stays in the ICU often develop neuromuscular weakness and flaccidity. Patients with poor forced expiratory volume, inadequate cough, or those who require a ventilator are also at increased risk. This risk increases as patients advance into later stages of the disease and have a breakdown of their cough and swallowing function. In PD, for example, the risk of being hospitalized for aspiration pneumonia is over three times higher than in healthy patients. Dysphagia in these populations often contributes to increased overall morbidity. Adults mostly develop overall swallowing muscle weakness that may become exacerbated by a neurologic decline, such as occurs in dementia or stroke involving certain aspects of the central nervous system (CNS). In adults, examples include acute and chronic stroke, dementia, amyotrophic lateral sclerosis, multiple sclerosis, Parkinson disease (PD), and Guillain-Barre syndrome. In pediatric patients, there is a strong correlation between recurrent aspiration pneumonia and swallowing dysfunction, specifically penetration, aspiration, reflux, and abnormal esophageal function. For instance, neuromuscular diseases may cause an overall weakness in swallowing solid foods, while cerebral palsy and other neurologically delaying syndromes cause difficulty with oral secretions and thin liquids. The mechanisms of aspiration differ in these. In children, the most common risk factors are encephalopathy, cranial nerve dysfunction (CHARGE – CN VII, IX, X), neuromuscular disease such as Duchenne muscular dystrophy, congenital muscular dystrophy, myotonic dystrophy, and spinal muscular atrophy as well as vocal fold immobility, and cerebral palsy. Several main risk factors include neurologic impairment, pulmonary diseases, supraglottic disease, and other conditions. Īnything contributing to the breakdown of the neuromuscular pathways involved in speaking, swallowing, breathing, and maintaining a patent airway can lead to chronic aspiration and its sequelae. Patients with dysphagia have triple the rates of pneumonia and suffer from a 2.9% increase in in-hospital mortality. In children, chronic pulmonary aspiration is one of the leading causes of death in neurologically impaired patients. It is the cause of significant morbidity and mortality in these populations. Chronic aspiration commonly affects three main demographics with specific comorbidities: children, elderly, and intensive care unit (ICU) patients. While aspiration can occur in healthy patients, repetitive and, thus, chronic aspiration indicates underlying pathology in the functioning of a healthy individual’s ability to speak, swallow, breathe, or maintain airway protection. The consequences of a single episode of aspiration vary from benign to catastrophic depending on the nature and volume of aspirated material. Chronic aspiration is most often secondary to microaspiration. :max_bytes(150000):strip_icc()/aspiration-pneumonia-4178835_color1-5c6f26e2c9e77c0001be5180.png)
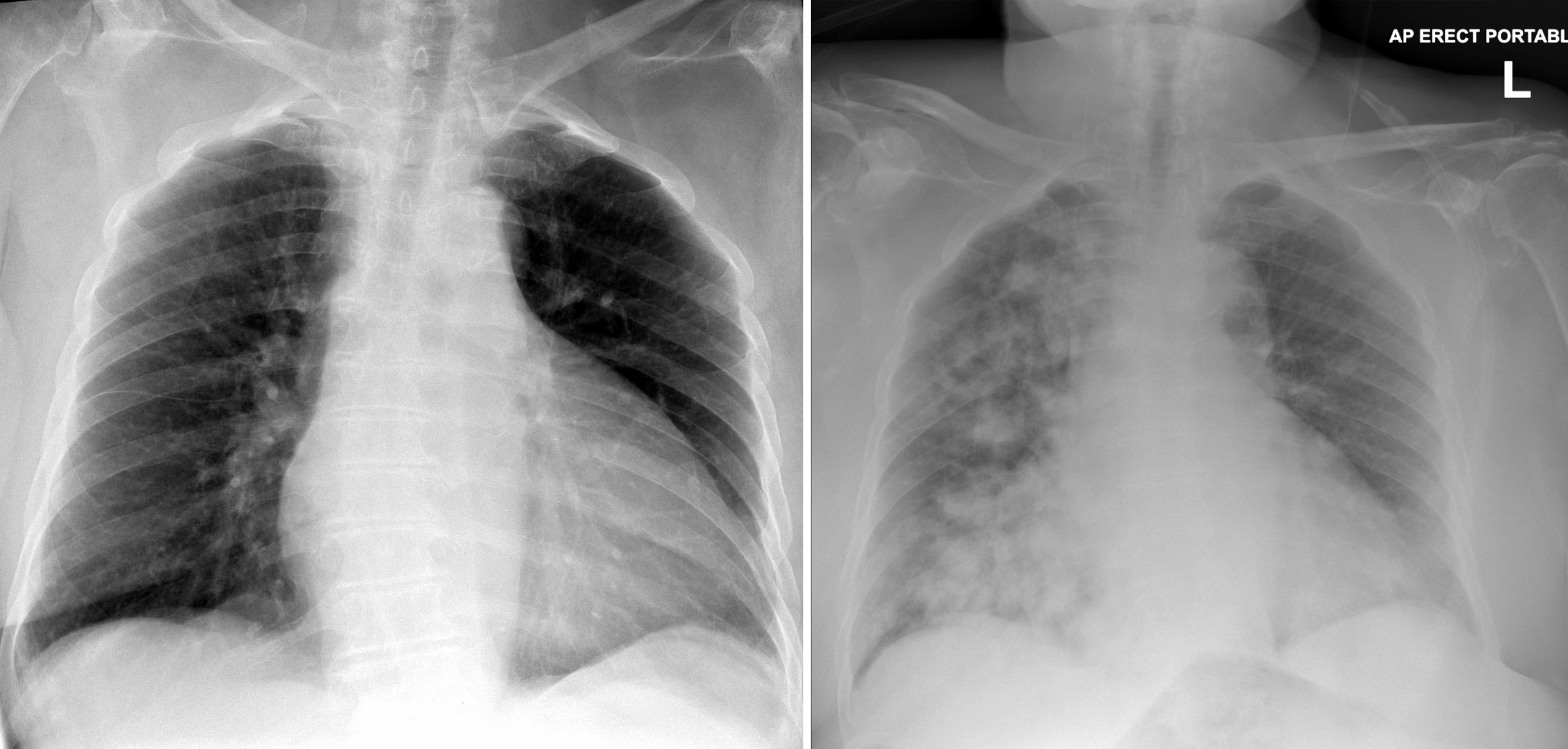
There is not a specific differentiating cut-off. Microaspiration occurs with minuscule amounts of foreign material are inhaled, while macroaspiration occurs when large amounts of foreign material are inhaled. 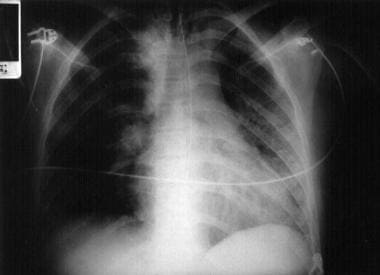
The term chronic aspiration refers to a common condition in the elderly population, pediatric patients with certain neurological disorders, and chronically intubated patients.Īspiration can be further classified into microaspiration and macroaspiration by the subjective amount of aspirate. Aspiration is a common problem that can occur in healthy or sick patients wherein pharyngeal secretions, food material, or gastric secretions enter the larynx and trachea and can descend into the lungs, causing an acute or chronic inflammatory reaction.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
